ACOs & DCEs
Supporting New Payment Models
CARAT helps streamline reporting requirements for Accountable Care Organizations (ACOs) and Direct Contracting Entities (DCEs) at the forefront of new CMS risk-sharing arrangements.
How CARAT Helps
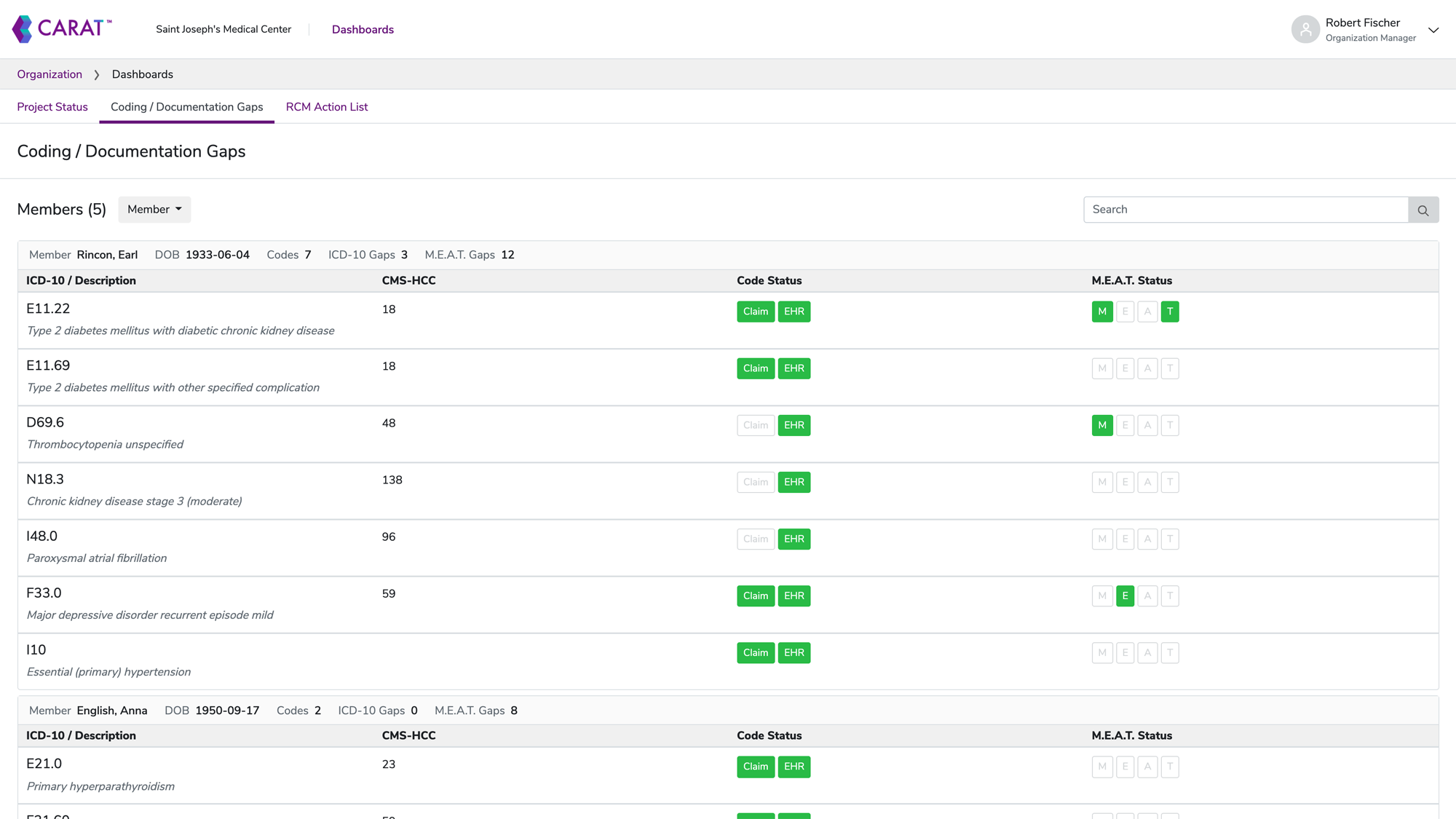
CARAT retrospectively reviews the clinical record to surface patient conditions and update the problem list, providing real-time suggestions within the EHR to close coding and documentation gaps or conduct a M.E.A.T. evaluation.
Real-time risk adjustment helps optimize claims during the encounter, completely eliminating the need for chase lists or patient recall.
-
-
-
- CARAT ProviderAssist
Retrospective and concurrent review provides action list to providers within the EHR to close coding and documentation gaps concurrent to the encounter. - CARAT Analytics
AI-powered intelligence analyzes and classifies the patient record, including data captured in PDFs, to support supplemental ICD-10 and HCC codes your team can use to correct claims. - Prospective Risk Adjustment
CARAT helps resolve under-documentation and under-scoring in real-time, evolving risk adjustment from a purely financial activity into a member-centric activity that supports care management.
- CARAT ProviderAssist
-
-
CARAT ProviderAssist
CARAT ProviderAssist provides a concurrent review of clinical documentation during each encounter, presenting coding and documentation gaps in real-time from within the EHR. CARAT ProviderAssist identifies the severity of each patient condition and encouraging actions to inform their care and support clinical documentation consistent with [M]onitoring, [E]valuating, [A]ssessing, [T]reating criteria (M.E.A.T.) for each HCC code in the patient record.
Prospective Risk Adjustment
A member-centered approach to risk
CARAT completely eliminates the need for chase lists, allowing ACOs and DCEs to optimize for risk and quality at the provider level in real-time.
AI-Powered Coding and Validation
CARAT analyzes clinical notes in the EHR concurrent to the encounter, helping to spot patterns and to suggest ICD-10 and HCC codes with higher accuracy.
Either immediately after the encounter, or as a final check by a coder, CARAT validates M.E.A.T. criteria and highlights any CDI opportunities to meet CMS guidelines. The entire process takes just 5 minutes a day, simplifying a time-consuming process.
CARAT Analytics
CARAT Analytics is a cloud-based analytics portal that supports your population health management efforts to monitor risk scores and identify gaps between documentation and ICD-10 and HCC codes. CARAT Analytics helps you stratify your population, drill down to the provider level, and stay on top of trends and opportunities.
Coding or M.E.A.T. gaps are automatically presented to the provider within the EHR with CARAT ProviderAssist, encouraging providers to take action to close gaps. Current and future encounters, supported by CARAT, encourage real-time validation of codes and M.E.A.T. criteria to eliminate chase lists.